Liver Condition Guide
Alcoholic Liver Disease (ALD)
Understanding alcohol-related liver damage — and the path to recovery.
Alcoholic Liver Disease encompasses a spectrum of conditions caused by chronic alcohol use, from simple fatty liver (steatosis) to alcoholic hepatitis and cirrhosis. The good news: early-stage ALD is reversible with sustained abstinence. LiverTracker helps you monitor your liver recovery, track sobriety milestones, and stay on top of critical lab values.

Understanding Alcoholic Liver Disease
ALD is the most common cause of advanced liver disease worldwide. It progresses through distinct stages — fatty liver, alcoholic hepatitis, fibrosis, and cirrhosis — each with different severity and reversibility. About 90% of heavy drinkers develop fatty liver, but only 10–20% progress to hepatitis or cirrhosis. The single most important intervention at every stage is complete alcohol abstinence.
Stages of Alcoholic Liver Disease
ALD progresses through a well-defined spectrum. Early stages are reversible; advanced stages require intensive medical management:
- •Alcoholic Fatty Liver (Steatosis): Fat accumulation in hepatocytes. Present in 90%+ of heavy drinkers. Fully reversible with 2–6 weeks of abstinence.
- •Alcoholic Hepatitis: Acute inflammatory injury. Ranges from mild to life-threatening. Maddrey DF ≥ 32 indicates severe disease requiring corticosteroids.
- •Alcoholic Fibrosis: Progressive scarring from repeated injury. May be partially reversible with sustained abstinence and nutritional support.
- •Alcoholic Cirrhosis: Irreversible scarring with portal hypertension. Complications include ascites, encephalopathy, variceal bleeding, and HCC risk.
- •Transplant Candidacy: For decompensated cirrhosis. Most centers require documented sobriety (typically 6+ months). Excellent outcomes post-transplant.
Symptoms & Warning Signs
Early ALD is often asymptomatic. Symptoms intensify as the disease progresses:
- •Fatigue, malaise, and general weakness
- •Nausea, loss of appetite, and unexplained weight loss
- •Right upper abdominal pain or tenderness
- •Jaundice (yellowing of skin and eyes) — indicates significant liver dysfunction
- •Abdominal swelling (ascites) — suggests portal hypertension
- •Confusion or personality changes (hepatic encephalopathy)
- •Easy bruising and bleeding — impaired coagulation
- •Spider angiomata and palmar erythema — classic signs of chronic liver disease
Risk Factors & Patterns
Not everyone who drinks heavily develops ALD. Risk factors beyond alcohol quantity include:
- •Duration and pattern of drinking (daily drinking worse than binge drinking for liver damage)
- •Women are more susceptible to ALD at lower alcohol intake than men
- •Genetic factors (PNPLA3, TM6SF2 gene variants increase susceptibility)
- •Concurrent obesity or metabolic syndrome (dual pathology with NAFLD/NASH)
- •Hepatitis C co-infection dramatically accelerates liver damage
- •Malnutrition — common in heavy drinkers, worsens liver injury
- •Iron overload — alcohol increases intestinal iron absorption
Treatment & Recovery
Abstinence is the cornerstone of treatment. Additional management depends on disease stage:
- •Complete alcohol abstinence — the single most important intervention at every stage
- •Nutritional rehabilitation: thiamine (B1), folate, zinc, magnesium, and adequate protein
- •Corticosteroids (prednisolone) for severe alcoholic hepatitis (Maddrey DF ≥ 32)
- •Lille Model at day 7 to assess steroid response — non-responders (>0.45) may need alternative treatment
- •Pentoxifylline as an alternative or adjunct to steroids in some protocols
- •Management of cirrhosis complications: diuretics for ascites, lactulose for encephalopathy, beta-blockers for varices
- •Liver transplant evaluation for those with decompensated cirrhosis and documented sobriety
- •Sobriety support: AA, SMART Recovery, counseling, and pharmacotherapy (naltrexone, acamprosate, baclofen)
Recovery & Prognosis
The liver has remarkable regenerative capacity, especially in early disease:
- •Fatty liver resolves within 2–6 weeks of abstinence in most patients
- •Mild alcoholic hepatitis: mortality <5% with abstinence and supportive care
- •Severe alcoholic hepatitis (DF ≥ 32): 28-day mortality 30–50% without treatment, improved with steroids in responders
- •Fibrosis can improve significantly over 6–12 months of abstinence
- •Compensated cirrhosis: 5-year survival >90% with abstinence, <70% with continued drinking
- •Decompensated cirrhosis: transplant may be the only curative option
- •Post-transplant 5-year survival for ALD exceeds 70%, comparable to other etiologies
Key Labs to Track
AST / ALT (De Ritis Ratio)
AST:ALT ratio > 2:1 is classic for ALD. A hallmark that distinguishes ALD from NASH.
GGT (Gamma-Glutamyl Transferase)
Highly sensitive to alcohol use. Elevated GGT with high AST/ALT ratio strongly suggests ALD.
MCV (Mean Corpuscular Volume)
Macrocytosis (high MCV) indicates ongoing alcohol use or B12/folate deficiency.
Bilirubin
Key component of MELD and Maddrey DF scores. Rising bilirubin indicates worsening liver function.
PT / INR (Prothrombin Time)
Measures coagulation. Essential for Maddrey DF calculation. Prolonged PT = impaired liver synthetic function.
Albumin
Low albumin reflects poor synthetic function and malnutrition — both common in ALD.
PEth (Phosphatidylethanol)
Objective alcohol biomarker. Detects drinking within past 3–4 weeks. Used by transplant teams.
CDT (Carbohydrate-Deficient Transferrin)
Elevated with sustained heavy drinking. Used alongside PEth for abstinence documentation.
Platelets
Low platelets suggest portal hypertension and advancing fibrosis/cirrhosis.
Creatinine
Key MELD component. Hepatorenal syndrome is a serious complication of advanced ALD.
How LiverTracker Helps
Track your Maddrey DF, MELD, and Child-Pugh scores automatically from uploaded lab reports
Monitor your De Ritis ratio (AST/ALT) and other ALD-specific markers over time
Celebrate sobriety milestones with our built-in sobriety tracker
Get AI-powered food scanning that flags hidden alcohol in foods and cooking ingredients
Receive personalized nutritional guidance for thiamine, folate, zinc, and protein recovery
Monitor GGT, MCV, PEth, and CDT trends as evidence of your liver's recovery
Access disease-specific AI chat that understands ALD, abstinence, and recovery
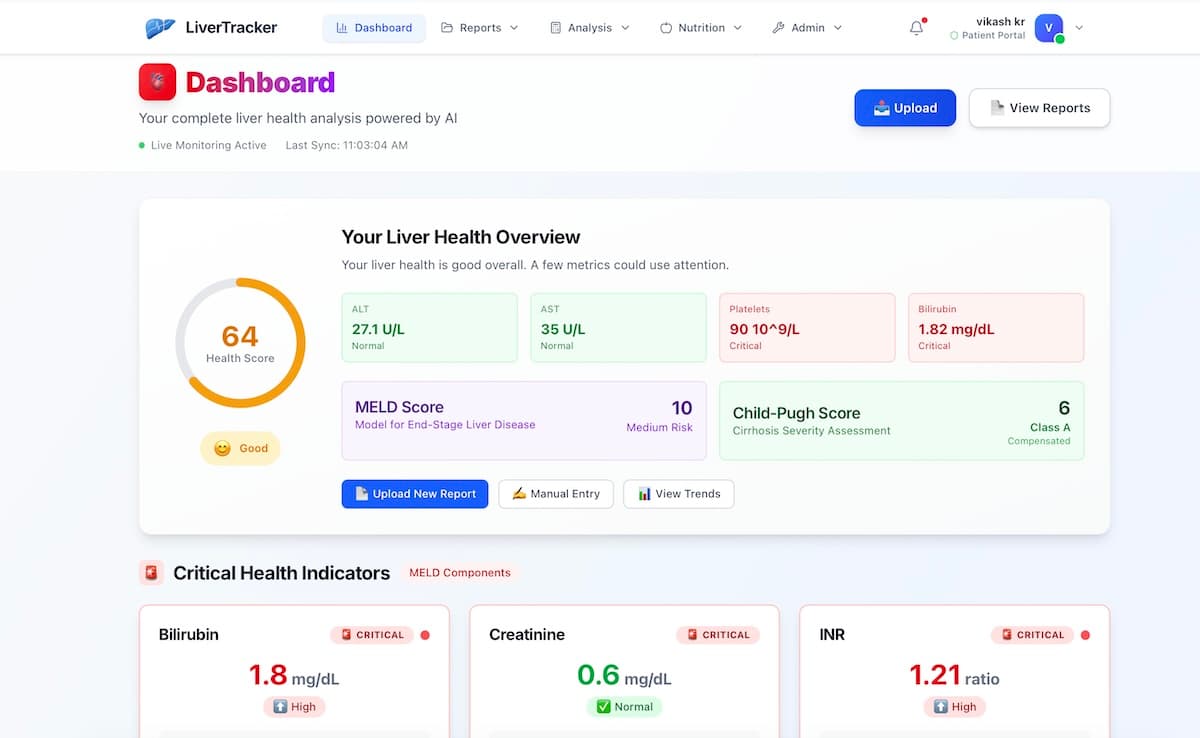
See Your Data Come to Life
Upload your lab reports and get instant AI-powered insights, trend charts, and health scores.
Frequently Asked Questions
Can my liver recover from alcoholic liver disease?
Yes — early-stage ALD (fatty liver) is fully reversible with sustained abstinence. Even fibrosis can improve significantly over 6–12 months of sobriety. Cirrhosis scarring is permanent, but abstinence prevents further damage, reduces complications, and dramatically improves survival.
What is the Maddrey Discriminant Function?
The Maddrey DF is a severity score for alcoholic hepatitis, calculated from prothrombin time and bilirubin. A score ≥ 32 indicates severe disease that may benefit from corticosteroid treatment. LiverTracker calculates this automatically when you upload your lab reports.
Can I get a liver transplant with ALD?
Yes. ALD is one of the most common indications for liver transplant. Most centers require a period of documented sobriety (typically 6 months), though some centers now consider early transplant for severe acute alcoholic hepatitis that doesn't respond to steroids.
How long does it take for the liver to heal after stopping drinking?
Fatty liver can resolve in 2–6 weeks. Inflammation (hepatitis) improves within weeks to months. Fibrosis regression takes 6–12+ months of sustained abstinence. GGT levels often normalize within 2–6 weeks, serving as an early indicator of liver recovery.
What is the De Ritis ratio and why is it important?
The De Ritis ratio is AST divided by ALT. A ratio greater than 2:1 is a classic hallmark of alcoholic liver disease. It helps distinguish ALD from other liver conditions and can indicate disease severity. LiverTracker tracks this ratio automatically over time.
What alcohol biomarkers do transplant teams monitor?
PEth (Phosphatidylethanol) detects alcohol use within the past 3–4 weeks and is the gold standard. CDT (Carbohydrate-Deficient Transferrin) detects sustained heavy drinking. EtG (Ethyl Glucuronide) can detect alcohol within 80 hours. These are used to objectively document abstinence for transplant eligibility.
Related Conditions
Take Control of Your Liver Health
Upload your lab reports, track your progress, and get AI-powered insights — all for free.
Get Started FreeMedical Disclaimer: This page is for educational purposes only and does not constitute medical advice. Always consult your hepatologist or primary care physician for diagnosis and treatment decisions.
